

A Trio of Exemplars of Medieval Islamic Medicine: Al-Razi, Avicenna and Ibn Al-Nafis
by Ritu Lakhtakia

The 1,000-year Legacy of Ibn Sina, Dr. Roy Casagranda & Museum of the Future’s Lessons from the Past
by Media Desk

This article has been produced from Chapter 6 "Contributions of Arab and Islamic Scholars to Modern Pharmacology" of the Book “Greco-Arab and Islamic Herbal Medicine: Traditional System, Ethics, Safety, Efficacy, and Regulatory Issues” by Bashar Saad and Omar Said, Copyright 2011 John Wiley & Sons, Inc.


Article Banner
From the beginning of time, history shows man’s reliance on natural products, varying from healthcare and basic needs to flavours and fragrances to name a few. This required the culmination of hundreds of wild plants, domestic animals and their respective by-products (e.g., bones, feathers, hooves, skins, and tusks) form important ingredients for the preparation of curative, and preventive medicine. The first records of the most important ingredients used in the preparation of curative and preventative medicine were from Mesopotamia dating from about 2600 BC. The best known Egyptian pharmaceutical record is the Ebers Papyrus dating from 1500 BC, which documents some 700 herbal and animal-based medicines including formulae. The earliest documented work from the Chinese materia medica dates from about 1100 BC (Wu Shi Er Bing Fang, containing 52 prescriptions), followed by works such as the Shennong Herbal (about 100 BC; 365 drugs), and the Tang Herbal (659 AD; 850 drugs). However, the Greeks contributed substantially to the rational development of the use of herbal medicines and other natural products. Around 300 BC, Theophrastus in his History of Plants, dealt with the medicinal qualities of herbs, and noted the ability to change their characteristics through cultivation. He was followed by Dioscorides (100 AD) who mentioned the collection, storage and use of medicinal herbs. Galen (130–200), who was renowned for his complex prescriptions and formulae used in compounding drugs, wrote around 30 books on the subject.
It is down to the organisational strengths and precise focus on multicomponent natural product preparations that Greco-Arab and Islamic medicine, Ayurveda, Kampo, and traditional Chinese medicine have flourished as systems of medicine in use for hundreds of years. Arab and Muslim scholars introduced hundreds of natural products, mainly medicinal plants and animal parts and products. They also developed a large and complex theoretical and practical knowledge in medicine, botany, and zoology with highly accurate precision and details. They introduced many new ideas and upgraded the knowledge about natural products and their potential pharmacological uses [1–3].
The currently available non-synthetic and/or semi-synthetic pharmaceuticals in clinical use are comprised of drugs derived from higher plants, followed by microbial, animal, and mineral products, in that order. This chapter highlights the importance of natural products as a source for new medicines as well as strategies used in selecting new potential natural products in Greco-Arab and Islamic medicine. This paper provides an overview of the development of natural drugs in Greco-Arabic and Islamic Medicine
Chapter 16 of the authors’ book discusses in detail the selection of potential natural products that were based on accumulated knowledge developed in the pre-Islamic period supported by a long history of trial and error that was then updated by new knowledge introduced by Muslim civilisation. These included natural products mentioned in the Holy Quran and in the Prophetic tradition. Foreign developments in medicine also became available to scholars through the translation of Greek, Indian, and Persian texts into Arabic. Additionally, throughout this period, physicians in the Islamic world introduced numerous innovative theoretical and practical ideas to the fields of medicine and pharmacy [1–3].
Medical knowledge in the Arabian Peninsula before Islam (610 CE) was folk medicine found in most human communities. We now know a lot about the nature of medicine practiced in Hejaz at that time from the Prophet’s medicine. The harsh environment, isolation in the desert, the nomadic Bedouin life, and the general illiteracy explain the low level of medical knowledge among Arabs before Islam. They used a wide variety of herbal and animal-based remedies. In general, they tended to live frugally, and to eat a simple diet. This may well have protected them against many diseases. Pre-Islamic Arabs used hijamah (cupping), kayy (cautery), and washim (branding with fire) (for details see Chapter 7 of the authors’ book). Among medical practitioners in the pre-Islamic era were Ibn Huzeem, Nadr Ibn Harith, and Ramtha al Tamiimi [3–5].


Drug discovery in Greco-Arab and Islamic medicine. Selection of potential natural products was based on (1) knowledge originated from traditional healers in the pre-Islamic period based on a long history of trial and error; (2) knowledge introduced by the Islam; (3) Greek and Persian medical knowledge; and (4) theoretical and practical knowledge introduced by Arab and Muslim scholars. At present, herbal-based drug discovery continues to provide new and important leads against various ailments, for example, cancer, psoriasis, diabetes, malaria, and pain. With only 5–15% of the approximately 300,000 species of higher plants systematically investigated, and the potential of the marine environment barely tapped, these areas will remain a rich source of novel bioactive compounds.
Many plants and animal products are mentioned in the Holy Quran and in the Hadith of the Prophet Mohammad (PBUH) (570–632), for example, dates, black seeds, olive leaf and olive oil, honey, and camel milk. These products were part of the everyday diet, as well as used for the treatment of various diseases. Later on these products were utilized in the Medicine of the Prophet (Al-Tibb al-Nabawi), which includes medical treatments, descriptions of diseases, prevention, health promotion, and spiritual aspects that were recommended by Prophet to his companions. Two Hadiths of the Prophet: “The one who sent down the disease sent down the remedy.” and “For every disease, Allah has given a cure” encouraged Muslims to search for possible remedies for each disease and greatly influenced the development of Greco-Arab and Islamic medicine during the Golden Age of the Arab–Islamic civilization.
The Book of Medicine (Kitab al-Tibb) of Sahih al-Bukhari (810–870) is recognized by the majority of Muslim scholars as one of the most authentic collections of what had been said and practiced (Hadith and Sunnah) by the Prophet. The scope of Prophetic medicine is discussed in the very well known commentaries of Sahih al-Bukhari by Ibn Hajar Al-Asqalani (d. 1449) and Abu Muhammad Al-‘Ayni (d. 1452), both were living in the Golden Age of the Arab–Islamic civilization, which witnessed the overlap of medical literature with other forms of science, literature, and culture. At the time, and influenced by these works, Prophetic medicine was understood to be relevant, not only during the life of the Prophet, but within their era and within their experience [6,7].
Prophetic medicine is not based on medical experiments but rather on inspiration and accumulated medical knowledge from ancient culture and tradition. According to a Hadith, the stomach is the core of the body and origin of many diseases:
“The stomach is the central basin of the body, and the veins are connected to it. When the stomach is healthy, it passes on its condition to veins, and in turn the veins will circulate the same and when the stomach is putrescence, the veins will absorb such putrescence and issue the same.”
Indeed, the Prophet used to recommend food for ailments (Table 1) even more than herbs or animal-based medicines. He used everything from barley soup to honey to camel milk to heal his followers and advised them to eat certain foods to prevent or cure other diseases. In fact, food is one of the oldest and most respected healing agents available to man. Honey, camel milk, dates, olive oil, and black seeds were the favoured foods by the Prophet who regarded food as part of an overall holistic approach. Concerning olive oil, he said:
“Eat olive oil and massage it over your bodies since it is a holy tree.”
Black seeds were regarded as a medicine that cures all types of diseases. He once stated:
“The black seed can heal every disease, except death.”
Dates are mentioned in 20 places in the Quran. Prophet is reported to have said:
“if anyone of you is fasting, let him break his fast with dates. In case he does not have them, then with water. Verily water is a purifier.”
To keep within the scope of this chapter we will discuss the therapeutic values of honey and camel milk. Traditional and medicinal values of black seeds, dates, and olive leaf and oil are discussed in Chapters 8 and 17 of the authors’ book.
Camel Milk: Camels milk which is rich in proteins and small peptides, plays a crucial role in innate immunity when transferred to offspring and may accelerate maturation of the immune system in newborns. It was the immune properties of these molecules that prompted investigators to assess their potential application in the prevention and therapy for newborns and adults, alike. For instance, lactoferrin exhibits antimicrobial, antifungal, antiviral, anti-parasitic, and anti-tumor activities.
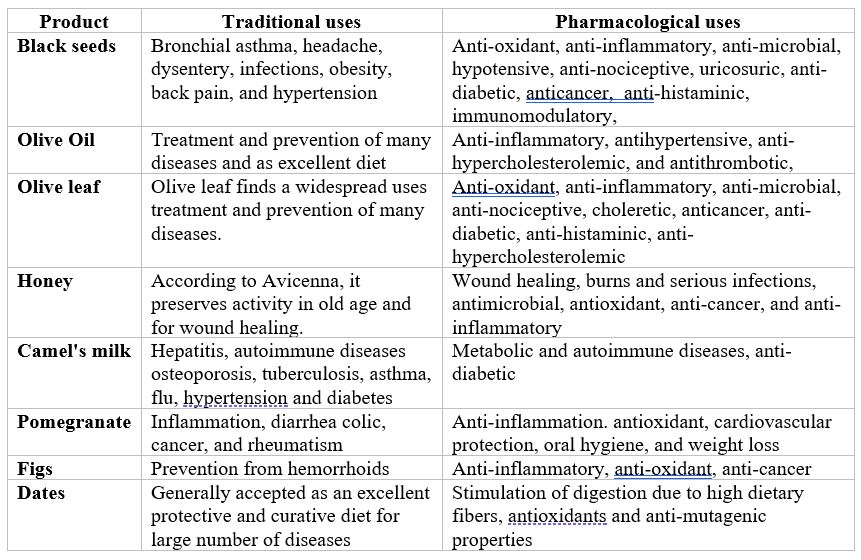

TABLE 1. Natural products used by Prophet Muhammad and their current pharmacological uses.
Lactoferrin is found in the intestinal epithelium, promotes bone growth, and accelerates the recovery of immune system function in immunocompromised animals. Casein is the predominant phosphoprotein that accounts for nearly 80% of proteins in cow milk. In fact, casein and casein-derived peptides showed protective activities in enamel demineralisation and as caries preventing agents. They were also protective in diabetic animals, reduced tumour growth, demonstrated antihypertensive activity, and diminished colic symptoms in infants. Glycomacropeptide, a peptide derived from kappa-casein, exhibited various antibacterial and antithrombotic activities. Alpha-lactalbumin demonstrated antiviral, anticancer, and antistress properties. Lysozyme found application in infant formulas, in treating periodontitis, and the prevention of tooth decay.
Camel milk is different from the milk of other ruminants; exhibiting low cholesterol, low sugar, high minerals (sodium, potassium, iron, copper, zinc, and magnesium), high vitamin A, B2, C, and E, low protein, and high concentrations of insulin. It has no allergic properties and it can be consumed by lactase-deficient persons and those with weak immune systems. Camel milk is considered to have medicinal properties. In the Sahara, fresh camel butter is often used as a base for medicines and it is used to develop medicines and cosmetics. Additionally, a series of metabolic and autoimmune diseases are successfully being treated with camel milk. In India, camel milk is used therapeutically against dropsy, jaundice, problems of the spleen, tuberculosis, asthma, anaemia, piles, and diabetes. A beneficial role of raw camel milk in chronic pulmonary tuberculosis patients has also been observed. In repeated clinical trials, it was observed that there was 30–35% reduction in daily doses of insulin in patients with type 1 diabetes who were treated with raw camel milk. The Prophet mentioned that camels milk and urine have medical effects, so Islam encourages and permits the drinking of camel milk and camel urine in case of necessary medical treatment. Bedouins treat many diseases and disorders with camel milk. This range from osteoporosis, rickets, hepatitis, digestive ulcers and disorders, spleen problems, tuberculosis, asthma, flu, and other respiratory diseases to controlling heartbeat, hypertension, and diabetes [6–8].
Honey (Detailed in Chapter 17 of authors’ book): A most glorified food since ancient times, honey has long been known. Often used as, an ingredient of flavoured drinks, a popular medicine and the principal-agent of liniments and plasters. It is frequently mentioned in early pharmacopeia, as an ingredient or carrier vehicle rather than a specific treatment. Dioscorides (40–80 AD) often mentioned honey as a vehicle for carrying therapeutic agents in de materia medicis. Hippocrates (460–377 BC), often cited as advocating honey for wound care, simply listed it as one of many ingredients in a multitude of unguents. Galen (130–200) recommended warming up the honey or cooking it, then using it to treat haemorrhoids and deep wounds. In the Muslim medical tradition, as in other medical traditions, including Ayurvedic, Chinese, and Roman, honey is considered as healthy drink. The Holy Quran describes its potential therapeutic value in Chapter The Bee, (Surah Al-Nahl) verse 69:
“……from within their bodies comes a drink of varying colours, wherein is healing for mankind, Verily in this is a Sign, for those who give thought.”
The Islamic Golden Age saw the rise of the use of honey in all its varying colours and forms for various ailments such as from swollen intestines, to inducing vomit (when a poison had been ingested), to skin disease, nerve injuries, lung diseases and tuberculosis, bladder wounds and possibly even for insomnia. In fact, Rhazes in his book, Al Hawi (Encyclopedia of Medicine), states:
“Honey is the best treatment for the gums. To keep the teeth healthy mix honey with vinegar and use as mouth wash daily. If you rub the teeth with such a preparation, it will whiten the teeth. Honey does not spoil and could also be used to preserve cadavers.”
Avicenna recommended using honey as part of an overall holistic approach to health that should be incorporated into daily diet to preserve and prolong life.
Due to side effects associated with the use of synthetic drugs, current research activities focus on alternative natural products as important source of therapeutic agents. Honey, has found to show important pharmacological benefits in the treatment/prevention of many diseases. Numerous of biological and pharmacological properties of honey have been noted including antibacterial, antifungal, anti-inflammatory, antioxidant, immunomodulatory, antiviral, wound healing, hepatoprotective, antidiabetic, hypoglycemic, and antihypertensive effects. These activities are the results of honey-derived compounds, such as phenols, flavonoids, vitamins, trace elements, proteins, amino acids, and sugars content. Honey was documented to exhibit inhibitory activity of carcinogenesis (initiation, proliferation, and progression) [9,10].
Pharmacological properties of honey include Anti-inflammatory, anti-bacterial, bio-stimulant, detoxifying effects, emollient, energetic, and nutritional
The development of Arab and Islamic medicine started with the Prophet. He was able to unite the Arab tribes who had been divided by revenge, rivalry, and internal fights. He created a strong nation who was able to defeat the Persian and Byzantine Empires. The Golden Age lasted roughly nine centuries—from the middle of the seventh to the end of the fifteenth century and in geographical terms covered nearly two-thirds of the known world.
The Muslim world was technologically and scientifically advanced. By the tenth century, their zeal and enthusiasm for learning resulted in the translation into Arabic of many important Persian, Indian, and Greek medical writings. The Caliph Al-Ma’mun in Baghdad became aware of what was to be learned from other civilisations, and therefore, he founded for this purpose, “The House of Wisdom”; a library and centre for the translation of texts into Arabic. Famous translators Hunayn ibn Ishaq and his colleagues translated numerous medical manuscripts by Hippocrates and Galen, philosophical works by Plato and Aristotle, and mathematical works by Euclid and Archimedes [1–4].


The House of Wisdom is a major Abbasid public academy and intellectual center in Baghdad Islamic Golden Age. It was library and centre for the translation of texts into Arabic. The scholars accumulated a great collection of world knowledge, and built on it through their own discoveries. (Archived)
The two phases that represent the Greco-Arabic medical system were the translation of Persian, Indian and Greek medical texts. During the second phase of the development, the scholars introduced their own medical theories and practices that became highly influential in Western science and teaching.
Like in other fields of science, the physicians developed innovative scientific methods for the field of medicine. This included the introduction of experimentation, quantification, experimental medicine, evidence-based medicine, clinical trials, dissection, animal testing, human experimentation and post-mortem autopsy by Muslim physicians, while hospitals in the Arab–Islamic world featured the first drug tests, drug purity regulations, and competency tests for doctors.
Arab–Muslim scholars were not guided by a long history of trial and error, but mainly by scientific methods, which has led to production of evidence-based medication. Avicenna discussed in his second book, on simple drugs (material medica), the nature and quality of drugs (see Chapter 7 of authors’ book), and the manner that compounding them influences their effectiveness. He stated:
“You can tell the potency of drugs in two ways, by analogy (qiyas) and by experiment (tajribah). We say experimenting leads to knowledge of the potency of a medicine with certainty after taking into consideration certain conditions.”
Avicenna then specified seven rules that need to be taken into account in the drug discovery process. These rules demonstrate the emphasis placed on evidence-based medication in the Greco-Arab medical system.
Examined closely, one may identify modern notions about testing drugs in each of Avicenna’s rules:
“Experiments should be carried out on the human body. If the experiment is carried out on the bodies of other animals it is possible that it might fail for two reasons: the medicine might be hot compared to the human body and be cold compared to the lion’s body or the horse’s body . . . The second reason is that the quality of the medicine might mean that it would affect the human body differently from the animal body.”
Currently, the development of new drugs is suffering from two major limitations. First, none of the animal species or in vitro test systems can properly mimic the complexity of the human body. A newly developed drug can induce unprecedented positive or negative biological effects involving systemic interactions specific to humans. This phenomenon was first described by Avicenna’s seventh rule and thus it remains relevant today. Second, systematic comparisons of drug studies done in animals and humans showed substantial differences, due to the failure of animal models to adequately mimic human disease (see Chapters 13 and 14 of the authors’ book for further discussion) [1–10].
Natural products can broadly be classified into three groups: Herbal-based, animal-based, or mineral-based products. It is believed that the vast majority of the world’s natural compounds have not been tested for their therapeutic value and that several novel sources of biodiversity are potentially available. These include a broader range of plant species than traditionally sampled, animals, marine organisms, and microbial diversity. Two examples of recently developed natural product-based drugs, one from a plant and one from an animal, deserve mention. Taxol, isolated from the Pacific yew, is a substance that kills cancer cells by a mechanism unlike that of other known chemotherapeutic agents: It prevents cell division by inhibiting the disassembly of the mitotic spindle. The discovery of the complex molecule taxol, and its novel mechanism of action, has led to the synthesis of several taxol-like compounds that are even more effective than the natural taxol. The other example that deserves mention are the peptide compounds in the venom of cone snails, a genus of predatory snails numbering about 500 species that inhabit tropical coral reefs. The diversity of these compounds is so great that it may rival that of alkaloids in higher plants and secondary metabolites in microorganisms. Some of these peptide compounds, which have been shown to block a wide variety of ion channels, receptors, and pumps in neuromuscular systems, have such selectivity that they have become important tools in neurophysiological research and may become invaluable to clinical medicine. One voltage-sensitive calcium-channel blocker, omega-conotoxin, binds with enormous specificity to neuronal calcium channels and has been found to have potent activity in animals both as an analgesic and as a means of keeping nerve cells alive following ischemia.
A re-evaluation of information presented on the sources of new drugs from 1981 to 2007 indicate that almost half of the drugs approved since 1994 are based on natural products. The list of recently approved natural product-based drugs include compounds from plants (elliptinium, galantamine, and huperzine), microbes (daptomycin) and animals (exenatide and ziconotide), as well as synthetic or semisynthetic compounds based on natural products (e.g., tigecycline, everolimus, telithromycin, micafungin, and caspofungin). They cover a range of therapeutic indications: anticancer, anti-infective, antidiabetic, among others [9–15].
Arab and Muslim scholars introduced hundreds of medicinal plants and developed a large and complex medical literature during The Golden Age of Arab–Islamic civilisation saw the introduction of hundreds of medicinal plants; as well as the development of a large and complex medical literature by Arab and Muslim scholars. These works explored and synthesised the theory and practice of medicine and botany with highly accurate precision and detail. They initiated many new ideas and upgraded knowledge about herbs and their potential pharmacological effects.
Al-Kindi (Alkindus) (800–873) introduced for the first time a scale to define the meaning of drug “degrees” in order to allow physicians to quantify the potency of their prescriptions. In addition, numerous encyclopaedias on botany were written, with highly accurate precision and detail concerning medicinal plants. For instance, Al-Dinawari (828–896) is considered to be the founder of Arabic botany for his Book of Plants, in which he described about 640 plants and described the phases of plant growth and the production of flowers and fruit. In 1161,
Ibn Abul-Bayan of Spain published The Bimaristan Law in Pharmacopoeia, Materitenses containing 607 detailed medications. Ibn Zuhr (Avenzoar), who lived in Seville (1091–1161), wrote the Al Kitab Al Jami, about liquids and creams. This book includes 230 medications that are mostly herbal, with a few of animal and mineral origin. This book gives a full description of the uses of herbs whether they are roots, seeds, or leaves. In the early thirteenth century, the Andalusian-Arabian biologist Abu al-Abbas al-Nabati published several books and dictionaries on the use of medicinal plants describing each plant species, the plant parts used, the preparation procedure used for each remedy, and the treatment procedure of certain diseases.
Ibn al-Baitar, who lived in Damascus, Syria (1197–1248), published The Book on Drinks and Foods, containing 260 references, it a most prestigious book in the Arabic pharmacopeia.
Al-Antaki (d.1599) described in his book 57 plants (about 79% of all the medicines mentioned) that were used as a source for simple drugs, or frequently as one ingredient in more complex herbal-based remedies. He described the plant and the way it was used by Greco-Arab and Islamic Arab physicians. Furthermore, Al-Antaki mentioned nonindigenous plants that were brought to the area specifically for their medicinal applications and described pharmacological uses of typical agricultural crops.
Al-Antaki was born blind in Antioch. Despite his disability, he became a famous pharmacist in the 16th century and learned many foreign languages (in addition to Arabic), including Greek. His life was dedicated to travelling across Turkey, Syria, and Egypt to seek knowledge. He finally resided in Egypt and worked as a senior pharmacist. Al-Antaki produced a number of medical books and his famous writing was entitled Tadhkirah or “Memorandum Book,” is still available today in bookstalls in Egypt in modern printings.
Selection Methods. In general, the correlation between morphological features, for example, size, shape, colour, texture, and taste of herbs and the anatomy of the affected organ led to the identification on new potential medicine. For instance, seeds with kidney shape are used for treating kidney stones, for example, Alhagi maurorum and Astragalus macrocarpus. Roots with shapes similar to the human body or fruits that resemble the human testis are used traditionally for stimulating sexual desire or treating sexual weakness. This doctrine of signatures is reflected in the usage of certain herbs, for example, the yellow decoction obtained from leaves of Rhamnus alaternus and the yellow juice from the fruits of Ecbalium elaterium are used for treating jaundice and liver diseases. For several herbs, the plant’s common name in Arabic refers to its medicinal applications [1–3, 11–15].


Drawings from Arabic manuscripts of the cultivated and the uncultivated kinds of the hindiba (Dwarf chicory, Cichorium pumilum). This plant is a well-known food and traditional remedy and it is well known in the Greco-Arab and Islamic herbal medicine as helpful in cleaning the body and supporting the liver. From left to right: Hindiba in an Arabic version of Dioscorides’ Materia Medica translated by Abdullah al-Huseyin b. Ibrahim al-Natili (Kitabu ‘l-khasa’is, Topkapi Museum Library, Ahmed III, MS 2127; Hindiba illustrated in Kitab min al-tibb fi ‘l-ahkami ‘l-kulliyyat wa’l-adwiya ‘l-mufrada, Suleymaniye Library, Ayasofya, MS 3748. See: Nil Sari (Source)
Current Strategies in Plant Selection. As discussed in detail in (Chapters 16 and 19 of the authors’ book) and the WHO guidelines (2003), complete taxonomical identification is an important factor during selection process. These include botanical identity, scientific name, including genus, species, subspecies or variety and family of the potential plant, and, if available, the local name should be verified. Furthermore, WHO guidelines highlight the importance of obtaining data regarding environmental conditions, such as soil, climate, and vegetation at the collection site. They also demand that a voucher specimen be deposited in a national or regional herbarium for authentication and further consultation by other researchers.
There are certain differences in approaches in selecting plants for industrial or rural applications. On one hand, the rural community applies natural products for treatment of common diseases. According to our recent survey, the majority of the Arab community in Palestine do use medicinal plants for treatment of common diseases such as diarrhoea, pneumonia, and wound infections and healing (Chapter 9 of authors’ book). On the other hand, the pharmaceutical industry requires medicinal plants for formulation of herbal-based remedies for commercial gain and hence focuses more on urban problems such as metabolic disorders, chronic diseases, and multidrug resistance with infectious pathogens. Whether for the rural community or for industrial application the selection of natural-based products should be based on their safety and effectiveness in prevention and/or treatment of a given illness. Currently, natural product selection generally follows five main routes:
1. Random Selection Followed by Chemical Screening: These so-called phytochemical screening approaches have been used in the past and are currently pursued mainly in developing countries. The tests are simple to perform, but false-positive and false-negative tests often render results difficult to assess. More important, it is usually impossible to relate one class of herbal-derived agents to specific biologic targets; for example, the alkaloids or flavonoids produce a vast array of biologic effects that are usually not predictable in advance.
2. Activity-Based Random Selection: Safety and efficacy of plant extracts are evaluated both in experimental animals and in vitro using cultured cells. During the last four decades, thousands of plant species have been screened in vitro and in vivo for several biologic activities, including anti-bacterial, anti-diabetic, anti-fertility, anti-fungal, anti-hypercholesteremic, anti-inflammatory, anti-tumor, cardiovascular, central nervous system depressant, cytotoxicity, diuretic, and others (see Chapter 8 of author’s book).
3. Ethnobotanical and Ethnopharmacological Studies: The ethnobotanical and ethnopharmacological approach uses information obtained from an ethnobotanical survey such as traditional medical uses, preparation techniques, geographical distribution of the plant, its abundance, whether it is threatened or endangered, a shrub or fast growing tree, easily cultivable, easily identifiable, and so on. Information such as the season of collection, parts that are used and whether those parts are seasonal and if there is any reported toxicity are also required. The information can be obtained from traditional medical practitioners and other experts such as village elders who are traditional users of medicinal plants. It is highly recommended that the ethnobotanical surveys are carried out by a team of botanists, traditional healers, and medical practitioners. In this manner the traditional healers would identify medicinal plants for treatment of different diseases, the botanist can carry out appropriate taxonomical and botanical characterisation of these medicinal plants, whereas the medical practitioners would help in proper identification of potential medical applications. These practitioners can help to evaluate whether an herbal remedy has curative properties, if it is merely alleviating the symptoms, or if it is exhibiting a placebo effect. However, information obtained from ethnobotanical surveys is not always reliable. It is possible that people may cite a particular plant more frequently since it is easily available, easily recognizable or resembles a certain disease feature. People may also mention plants about which they have gained information from personal communication, books, from the media, or from the internet. In addition, publications concerning medicinal plants are often compilations from other texts and seldom stem from personal experience, making evaluation difficult.
4. Knowledge Obtained from Ancient Medical Systems: A huge amount of medical information is available in ancient texts from different sources such as Greco-Arab and Islamic medicine. However, while studying ancient medical texts, one must consider the fact that the plants may have evolved over a period of time resulting in changes in their phytochemical composition and hence their medicinal properties and therefore validation is required. Nevertheless, the success rates of the traditional-based approaches are substantially higher than those of random screening since the continued use of crude preparations are, in fact, comparable to small scale clinical trials. In general, the search for the medicinal plants can follow three main routes: random, ethnobotanical, and ethnopharmacological, traditional knowledge obtained from ancient medical systems, and ecological search.
5. Ecological Approach: Pharmacologically active plants can also be identified using an ecological approach. The absence of predation in areas infested with herbivores, for example, can indicate the presence of toxic compounds. Selection can also be based on an approach called zoopharmacognosy, a variation to the ecological approach, which proposes the selection of plant species regularly ingested by animals, mostly primates for reducing pain, microbial or worm infestations.
The treatment of human ailments by using medicines that are obtained from animals or ultimately are derived from them is known as zootherapy. Animal-based medicines have been elaborated from parts of the animal body, from animal metabolites (corporal secretions and excrements), or from animal products (nests and cocoons). Data have been found on such usages in ancient civilizations, such as Egypt and Mesopotamia, which left their mark on the various civilizations that later arose in these regions. Historical sources of ancient Egypt mention the medicinal uses of animal-derived products, such as, bee honey, cattle milk, ox organs, lizard blood, bat limbs, ambergris from the sperm whale, and the glands of the musk deer.
Historical scripts of civilizations of ancient Mesopotamia, mainly the Assyrian and the Babylonian, contain descriptions of beeswax and honey, mongoose blood, turtle shell, fish oil, goat skin, bird excrement, and animal fat. In India, the Hindu religion has used five products of the cow for purification since ancient times. In ancient China, among many other substances of animal origin, the glands of the musk deer were used.
Hippocrates (460–377 BC) used among many other animal substances cattle milk, chicken eggs, mammal horns, and sea sponge as remedies. About one-tenth of the remedies mentioned in Dioscorides’s (100 AD) Materia Medica were animal parts and products. The ancient Jewish scripts mention several animals and their medical uses: honey was used to treat bulimia and goat milk was used to cure coughing. Snakes, human urine, pearls, mammal glands, and several other substances were used for their therapeutic effects.
Zootherapy in Greco-Arab and Islamic Medicine. Medieval Greco-Arab and Islamic literature offers a huge amount of data about natural products in general, with emphasis on herbal as well as animal-based remedies in particular. As discussed in (Chapter 7 of the authors’ book), the medicine of the Prophet (tibb al-nabawi) indicates intensive medicinal use of milk, cattle cheese, and bee honey.
Early Arab and Muslim physicians such as Rhazes (864–930), Avicenna (980–1037), Al-Kindi (800–873), and Al-Antaki (d. 1599), prescribed many animal-based remedies. These included camel milk, cattle fat, coral, crab, dog, fish stone, horse, lizard, medical skink, mouse, pearl, pigeon, rabbit, rhino and goat horns, scorpion, snake, squid, turtle, and wolf, and animal products such as honey, wax, milk, and eggs. About 10% of all the medicinal substances used in the Arab–Islamic world during the Middle Ages were of animal origin.
Most animal products, such as milk, cheese, and honey, were used in the diet for the prevention and treatment of various diseases, which chapter 17 of the authors’ book discusses in detail.
Detailed information on animals and animal-based products are found in various encyclopaedias such as Daud al-Antaki’s book, Tadhkirat Uli l-al-Bab wa l-Jami li-L-‘Ajab al-‘Ujab, and Hayat al-Hayawan (life of animals) by Al-Damiri (1344–1405), an Egyptian zoologist. The latter is one of the most well-known medieval works on zoology and animals. The work is a compilation of over 500 prose writers and nearly 200 poets. The correct spelling of the names of the animals is given with an explanation of their meanings.
The use of the animals in medicine, their lawfulness as food and their position in folklore are the main subjects explained, alongside long, irrelevant stretches of political history. Al-Damiri describes in his lexicon hundreds of animals, tens of which were used as remedies.
One of the most important sources for learning about medicinal substances of natural origin used among physicians and inhabitants of the Bilad al-Sham (Bilad al-Sham is the medieval Arabic name for a large area including the majority of present-day Syria, Israel, Lebanon, and Jordan also known as the Levant) is the work of the physician, Daud al-Antaki, who lived and practiced during the second half of the sixteenth century. Al-Antaki’s book, Tadhkirat Uli l-al-Bab wa l-Jami li-L-‘Ajabal-‘Ujab, is a medical and pharmaceutical encyclopaedia, containing detailed descriptions of natural-based remedies in use in the Bilad al-Sham. This four-part book begins with an introduction to the four parts where he lists the sciences addressed in the main body of the work and explains the connection of each to medicine. Part one is a general preface on medical wisdom and discusses various diagnostic methods.
Al-Antaki opens part two with a historical survey of the development of pharmaceutical science, beginning with Dioscorides and ending with Al-Antaki’s contemporaries. This part of the text also describes the nature of simple and complex drugs and gives general instructions to pharmacists. Part three lists medicinal substances in Arabic alphabetical order and describes their application as well as their use as an ingredient in complex drugs. The list includes hundreds of plants, minerals, and animals (and their organs). Part 4 describes diseases, their causes and symptoms, and various specific treatments.
Animal-Based Remedies: A remarkably wide range of animals and their parts were used therapeutically in the medieval era. Physicians, pharmacists, and patients alike, used a remarkably wide range of animals and their parts for therapeutic benefits. These included (1) wild animals such as: ant, bee-eater, cuttlefish, desert partridge, earthworm, fish, firefly, flycatcher, fox, frog, gazelle, hedgehog, lizard, scarabee, scorpion, seashell, and snail; (2) domesticated animals such as: ass, cattle, hen, honey and wax, goat, goose, lamb, mule, and silkworm; (3) parasites of humans or domesticated animals such as: louse, mouse, and stinkbug; (4) rare animal substances such as: adder, bustard, coral, kermes, lacca, ostrich, triton, and squid. These animals were hunted in season or collected in the desert, on the seashore, or in remote areas; (5) exotic animal substances such as: common beaver, musk, pearl, Spanish fly, sperm whale, which were imported from distant lands via the trade routes and therefore were exotic.
Animal substances were utilized to treat a broad spectrum of symptoms and diseases such as skin diseases, bleeding, wounds, internal disease, haemorrhoids, animal bites, and sex-related diseases. Al-Antaki described in his book the therapeutic benefits of a number of animals and their products. Accordingly, the cow cheese was used to treat scabies, to relieve burning sensations in the urinary tract, to treat kidney problems, and as an aphrodisiac. The internal organs of the mule were used as painkillers and to prevent inflammation of the joints. Eating a mule’s heart was supposed to purify the body, eating its liver prevented pregnancy, and drinking its urine stopped excessive tears. The silkworm with its many medicinal properties, was used in the following ways, its ashes were used to treat wounds; its liquids were used to eliminate scars; whereas its boiled body was used to treat swellings, throat infections, and racing heartbeat.
The stinking bug, a common parasite at that time, was used to treat headaches, uterine problems, coughing, and fever, to dissolve kidney stones, and to open a blocked urinary tract.
Al-Antaki mentioned three wild birds: the bee eater, the flycatcher, and the bustard. The bustard’s flesh, fat, blood, and internal organs (such as the stomach), ashes from its feathers, its eyes, and claws were used to prevent or eliminate phlegm, treat pneumonia, dissolve kidney stones, and remove cataracts. Products of the flycatcher were used as a drug to dissolve blood clots, to treat jaundice and infected spleens, to dissolve kidney stones, and to cure eye and skin diseases. The bee-eater was used to eliminate odour, treat colds and skin diseases, and remove phlegm. The firefly is identified as possessing special medicinal properties and was used to dissolve kidney stones and to heal haemorrhoids.
Theriak (theriac), a mixture of many plants, poisonous minerals, and extracts of animals generally poisonous such as snakes and scorpions, was used as an antidote to snake bites, scorpion stings, animal bites, and poisoning by different kinds of poisons.
Many of the animals were mentioned in historical scripts of the Greco-Arab and Islamic world are currently still in use in traditional medicine in the Arab and Islamic world. For instance, to name a few, in Iraq 12 kinds of animals are described as medicinal sources, Similarly, surveys conducted in Syria during the 1970s found that about 5% of the natural remedies sold in the markets were animal based. A survey of traditional medicines in use in the markets of Israel recorded 20 substances of animal origin. Similar data are derived from surveys conducted in Jordan.
In Pakistan, for instance, 31 animal parts and products are used, constituting 9% of all the medicinal substances used in traditional medicines. A survey of traditional medicines in use in the markets in Sudan has recorded 23 animals that are used as sources of remedies in Sudanese traditional medicine.
Current Trends. Leeches are undergoing a triumphant resurgence in medicine, particularly in microsurgery. Traditionally, leeches are usually used in conditions such as abnormal swellings, piles, inflammatory abscess, skin diseases, rheumatoid arthritis, eye diseases, poisonous bites, erysipelas, and so on. The first recorded use of leeches in medicine was in 200 BC by Greek physicians and was later reintroduced by Avicenna in The Canon of Medicine. Leech therapy became a popular practice in medieval Europe, namely the leeches from Portugal and France, due to the influence of The Canon.
Like Avicenna, Abu al-Qasim al-Zahrawi (known as Albucasis 936–1013) recommended the use of leeches on parts of the body for which application of cupping-vessels is impossible, either because of part is bare of flesh, like the nose.
A more modern use for medicinal leeches was introduced by Abd el-Latif al-Baghdadi in the twelfth century, who wrote that leeches could be used for cleaning tissues after surgical operations. He did, however, understand that there is a risk over using leech, and advised patients that leeches need to be cleaned before use and that the dirt or dust “clinging to a leech should be wiped off” before application. The revival of interest in leech therapy was caused due to the unsatisfactory results of conventional treatment of many cardiovascular diseases, and to new findings about the leech’s salivary components and its influence on the human organism. During the blood-sucking process, leeches produce an anticoagulant, a local anaesthetic, a vasodilator, and an antibiotic, all of which are useful to their blood-sucking propensities and are capable of being turned into therapeutic advantage. Leech secretions are more effective than heparin at inhibiting fibrin formation because, being smaller, they penetrate the clot more effectively. Also, whereas heparin acts indirectly by activating the anticoagulant antithrombin III, leech anticoagulants inhibit specific steps in the coagulation cascade.
One of the best-known examples of a successful animal-based drug is that of the angiotensin-converting enzyme (ACE) inhibitor, a component of snake venom (Bothrops jararaca). This enzyme is responsible for converting an inactive precursor into the locally active hormone angiotensin, which causes blood vessels to constrict and hence raises blood pressure. By pharmacologically blocking the enzyme’s activity, blood pressure can be reduced, and agents with this activity are commonly used to treat people with hypertension. Currently, ACE inhibitors like captopril, enalapril, and lisinopril are among the top 20 best-selling medicines in the world.
Several compounds have been extracted from fish and these are employed as remedies in the medical cannon. Today, some of these compounds are important as tools for biochemical research or as new leads for the development of anticancer and antiviral drugs. Oily fish, like cod, herring, salmon, and turbot, have a great medicinal value to human beings due to a polyunsaturated compound known as Omega-3. This substance helps the prevention of arthritis. The presence of an anticoagulant system in the plasma of Atlantic salmon (Salmo salar) and rainbow trout (Oncorhynchus mykiss) has been confirmed; similarities exist with the protein C found in the mammal anticoagulant system. Tetrodotoxin (TTX), a water-soluble guanidinium derivative, is an example of a bioactive compound produced by marine organisms such as the puffer fish that resembles procaine in its ability to inhibit transmission of nerve cells. When diluted it acts as an extraordinary narcotic and analgesic.
Amphibians have provided compounds that demonstrate a therapeutic advantage. Peptides extracted from the scraped secretions of Phyllomedusa bicolor, for instance, are used in the treatment of depression, stroke, seizures, and cognitive loss in ailments such as Alzheimer’s disease. Some of these compounds are important tools for biochemical research or as new leads for the development of anticancer or antiviral drugs. The number and diversity of compounds produced by amphibians in their granular glands is surprisingly high, even within single species. The main categories of secretions include biogenic amines, bufogenines and bufotoxins (steroids), alkaloids and peptides (including smaller oligopeptides, polypeptides, and proteins), and the as yet uncharacterized zetekitoxins found in the Middle and South American harlequin frogs, genus Atelopus. Most alkaloids of amphibian skin appear to be sequestered from dietary arthropods.
Many of the compounds contained in granular gland secretions have a defensive role. Their pharmacological effects include cardiotoxic, myotoxic, and neurotoxic activities, some are vasoconstrictive and hypotensive agents while others have hallucinogenic effects—all properties that would adversely affect a potential predator. Dermmophin, a novel opioid heptapeptide produced in the skin of the South American leaf frogs, genus Phyllomedusa, has a 1000-fold greater effect than morphine at the same concentration. It is therefore possible that molecules derived from amphibian sources might provide useful alternative or supplementary treatments, primarily as antimicrobial and antifungal agents. The presence of a wide range of peptides with unknown properties enhances the prospects of using peptide vaccines for viral diseases.
Insects have proven to be very important as sources of drugs for modern medicine since they have immunological, analgesic, antibacterial, diuretic, anaesthetic, and anti-rheumatic properties. Chitosan, a compound derived from chitin, has been used as an anticoagulant and to lower serum cholesterol level, as well as to repair tissues, and even in the fabrication of contact lenses. The major component of bee venom, the tetrameric polypeptide melittin, may be responsible for the often-reported anti-arthritic and anti-inflammatory effects. A toxin named margatoxin has been isolated from the venom of the scorpion Centruroides margaritatus. This chemical compound blocks lymphocyte activation and the production of interleukin-2 by human T-lymphocytes.
The Merck Company has filed a patent application for the use of margatoxin as an immunosuppressant, which may be potentially useful in treatment of autoimmune diseases or in preventing the rejection of organ transplants. The use of animal toxins to determine nerve action mechanisms could prove to be the starting point for designing new treatments for Alzheimer’s disease [11–17].
Minerals and Metals: Al-Antaki described five minerals that were used medicinally. Like many other early writers, he discussed the use of asphalt in medicine. (1) Asphalt, (2) Jew’s Stone, (3) Iron Rust, (4) Dry Earth, (5) Hematite.
Friedrich Sertürner (1783-1841), a German pharmacist and a pioneer of alkaloid chemistry, isolated the first pharmacologically active pure morphine compound from opium produced by cut seed pods of the opium poppy (Papaver somniferum) He initiated an era wherein drugs from plants could be purified, studied, and administered in precise dosages that did not vary with the source or age of the material (e.g., plant).
Pharmaceutical research expanded after the Second World War to include massive screening of microorganisms for new antibiotics following the discovery of penicillin. By 1990, about 80% of drugs were either natural products or analogs inspired by them. Antibiotics (e.g., penicillin, tetracycline, erythromycin), antiparasitics (e.g., avermectin), antimalarials (e.g., quinine, artemisinin), lipid control agents (e.g., lovastatin and analogs), immunosuppressants for organ transplants (e.g., cyclosporine, rapamycins), and anticancer drugs (e.g., taxol, doxorubicin) revolutionized medicine. Life expectancy in much of the world lengthened from about 40 years early in the twentieth century to more than 77 years today.
As discussed above, natural products have provided the inspiration for most of the active ingredients in drugs: about 80% of medicinal products up to 1996 were either directly derived from naturally occurring substances or were inspired by a natural product. In an extensive review of new drugs introduced between 1981 and 2002, 28% of the 868 new chemical entities were natural products or derived from natural products, with another 24% created around a pharmacophore from natural substances. In addition to launched products, at least 70 natural product-related compounds were involved in clinical trials in 2004, and exploration of the bioactivity of natural products continue to provide novel chemical scaffolds for further drug discovery.
Various reasons have been put forward to explain the success of natural products in drug discovery: their high chemical diversity, the effects of evolutionary pressure to create biologically active molecules, the structural similarity of biomolecular targets across many species, and so on. Evidence for many of the suggested explanations is hard, if not impossible to obtain. However, analysis of the structural diversity of natural products does support the belief that collections of natural products are not only more varied than those made up of synthetic compounds, particularly those produced by combinatorial chemistry, but also that natural products are more similar than synthetic compounds to the “chemical space” occupied by drug molecules.
Further analysis of the structural features of natural products has led to ways to describe the regions of chemical space they occupy. From such approaches, it may be possible to guide the synthesis of libraries of new molecules that will occupy parts of chemical space predicted to be associated with drug-like biological activity.
Although the expansion of synthetic medicinal chemistry in the 1990s caused the proportion of new drugs based on natural products to drop to about 50%, 13 natural product-derived drugs were approved in the United States between 2005 and 2007, with five of them being the first members of new classes. With such a successful record, it might be expected that the identification of new metabolites from living organisms would be the core of pharmaceutical discovery efforts. However, many pharmaceutical firms have eliminated their natural product research during the last decade. Although more than 100 natural product drugs are currently undergoing clinical trials and at least 100 similar projects are in preclinical development, this represents about a 30% drop between 2001 and 2008. This is because of the perceived disadvantages of natural products (e.g., difficulties in access and supply, complexities of natural product chemistry and inherent slowness of working with natural products, and concerns about intellectual property rights), and the hopes associated with the use of collections of compounds prepared by combinatorial chemistry methods [13–17].
1. Saad B, Azaizeh H, Said O. Arab herbal medicine. In: Watson RR, Preedy VR (Eds.), Botanical Medicine in Clinical Practice. CABI, Wallingford, UK, 2008.
2. Saad B, Azaizeh H, Said O. Tradition and perspectives of Arab herbal medicine: a review. eCAM 2005; 2:475–479.
3. Saad B, JadAllah R, Daraghmeh H, Said O. Medicines and method of therapy in the Arab and Islamic. Med. Int. J. Biosci. Biotechnol. Res. Commun. 2009; 2:123–132.
4. Oumeish Y O. The philosophical, cultural, and historical aspects of complementary, alternative, unconventional, and integrative medicine in the old world. Arch Dermatol. 1998; 134:1373–1386.
5. Pormann P E, Savage-Smith E. Medieval Islamic Medicine. Edinburgh University Press, 2007.
6. Syed I B. Spiritual medicine in the history of Islamic medicine. JISHIM 2003; 2:45–50.
7. Deuraseh N. Health and medicine in the Islamic tradition based on the book of medicine (Kitab Al-Tibb) of Sahih Al-Bukhari. JISHIM 2006; 5:2–14.
8. Imtara H, Kmail K, Touzani S, Khader M, Hamars H, Saad B, Lyoussi B (2019) Chemical analysis, cytotoxic and cytostatic effects of twelve honey samples collected from different regions in Morocco and Palestine, Evidence based complementary and alternative medicine Volume 2019, Article ID 8768210, 11 pages.
9. Touzani S, Embaslat W, Imtara H, Kmail A, Kadan S, Zaid H, ElArabi I, Lyoussi B, Saad B, (2019) “In Vitro Evaluation of the Potential Use of Propolis as a Multitarget Therapeutic Product: Physicochemical Properties, Chemical Composition, and Immunomodulatory, Antibacterial, and Anticancer Properties,” BioMed Research International, vol. 2019, Article ID 4836378, 11 pages, 2019.
10. Zimecki M, Kruzel ML. Milk-derived proteins and peptides of potential therapeutic and nutritive value. J. Exp. Therapeut. Oncol. 2007;6(2):89–106.
11. Ibn Sena (Avicenna), Al Qanun Fi al Teb, Book 8. Dar Alfiker, Bairut, Lebanon, 1994, pp. 77–78 (in Arabic).
12. Al-Antaki D. Tadhkirat Uli l-al-Bab wa l-Jami li-L-‘Ajab al-‘Ujab. Cairo, 1935 (in Arabic).
13. Lev E. Traditional healing with animals (zootherapy): medieval to present-day Levantine practice. J. Ethnopharmacol. 2003; 85:107–118.
14. Cragg G M, Newman D J. Biodiversity: a continuing source of novel drug leads. Pure Appl. Chem. 2005;77(1):7–24.
15. Costa-Neto E M. Animal-based medicines: biological prospection and the sustainable use of zootherapeutic resources. An. Acad. Bras. Cienc. 2005;77(1):33–43.
16. Li J W-H, Vederas J C. Drug discovery and natural products: end of an era or an endless frontier? Science 2009;325(5937):161–165.
17. Harvey A L. Natural products in drug discovery. Drug Discov. Today 2008;13 (19–20):894–901.
***


Bashar Saad, PhD, is Professor of cell biology and immunology at the Arab American university in Jenin, Palestine, and at Al-Qasemi Academic College, Baga Algharbiya, Israel. He made a significant contribution in combining cell biology, immunology, and 3D cell culture techniques with Arab-Islamic herbal wisdom. His research interests include antidiabetic, anti-inflammatory and anticancer properties of medicinal plants. He has written more than 150 original papers as well as review articles and book chapters on Arab-Islamic herbal medicine.
***


Omar Said, Phd, is the Chief Research Officer and founder of BeLeaf Pharma. He is a pioneer in the field of Greco-Arab medicine, herbal medicine and pharmacology. He serves as the head of the Arab medicinal plant project in the Galilee Society R&D regional centre, Israel. He has a PhD in Pharmacology. As an expert in the fields of pharmacology and ethnopharmacology, he made a significant contribution in combining this modern science with the medicinal plants’ tradition. His research interests include diabetes, obesity, fertility, psoriasis, acne, hyper-lipidemia, and liver diseases. He has written more than 65 original papers as well as review articles and book chapters on Arab-Islamic herbal medicine.
4.7 / 5. Votes 9
No votes so far! Be the first to rate this post.






Muslim Heritage:
Send us your e-mail address to be informed about our work.
This Website MuslimHeritage.com is owned by FSTC Ltd and managed by the Foundation for Science, Technology and Civilisation, UK (FSTCUK), a British charity number 1158509.
© Copyright FSTC Ltd 2002-2020. All Rights Reserved.
